[Voice] Should euthanasia be legal?
As the government looks to change the law on life-prolonging treatment...
By Korea HeraldPublished : Aug. 19, 2013 - 20:11
If there is a right to life, is there also a right to die? That is the question the National Bioethics Committee sought to answer in a recommendation at the end of July that terminally ill patients and their family be given the right to withdraw life-prolonging treatment in certain circumstances.
The proposal, which would apply only to patients close to death with no chance of recovery, would end the current legal obligation on doctors to provide all treatment necessary to sustain life irrespective of the patient or their family’s wishes. The recommendations, which would have to pass the National Assembly to acquire legal force, also propose that patients be encouraged to document their wishes regarding treatment in the event they are unable to give consent. Where a patient is unable to make health care decisions for himself and his wishes are unclear, the family would be allowed to cease treatment by unanimous agreement.
The proposal, which would apply only to patients close to death with no chance of recovery, would end the current legal obligation on doctors to provide all treatment necessary to sustain life irrespective of the patient or their family’s wishes. The recommendations, which would have to pass the National Assembly to acquire legal force, also propose that patients be encouraged to document their wishes regarding treatment in the event they are unable to give consent. Where a patient is unable to make health care decisions for himself and his wishes are unclear, the family would be allowed to cease treatment by unanimous agreement.
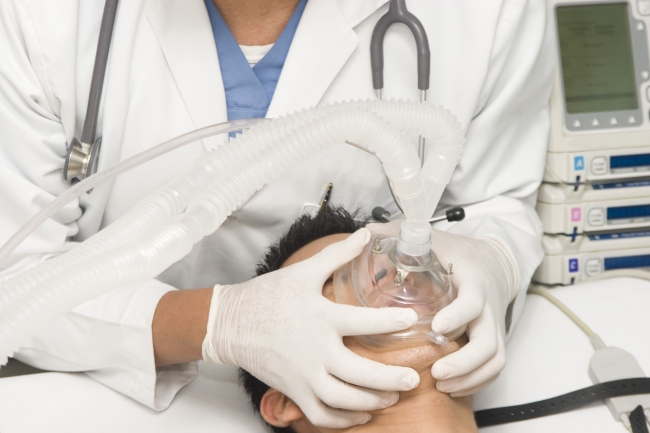
The withdrawal or withholding of life-sustaining treatment is widely defined as “passive” euthanasia, as opposed to its “active” equivalent where action is directly taken to end life.
Contested definition
An official from the Ministry of Health and Welfare, however, insisted that what was proposed did not meet the definition of euthanasia in any sense.
“As euthanasia will not be legalized in Korea, I will answer the question in terms of whether to continue treatment or not,” Cho Gui-hoon, a senior official at the department of bioethics policy, told The Korea Herald.
“First, the question of continuing treatment or not will follow the patient’s own decision first and if it is not clear, the decision will be based on the family members’ agreement and other factors.”
He added that euthanasia, under his definition, would not be legalized in the foreseeable future.
Cho also indicated that the specifics of the proposals were still open to scrutiny and could be revised.
“During the legalization process, more discussion is needed with patients’ organizations and religious groups before reaching the final decision,” he said. “Currently, there is nothing decided on how to prevent side effects of the law such as collusion between family members and doctors.”
In the face of a legislative vacuum, Korea’s medical community has implemented its own guidelines on the so-called right to die. Under the Korean Medical Association’s code of ethics, doctors are permitted to withhold life-prolonging treatment at the request of a patient. But these guidelines are without legal basis, leaving doctors caught between the law and their patients’ wishes, according to Park Han-son, a psychiatrist at Saint Andrew’s Neuropsychiatric Hospital in Icheon, Gyeonggi Province.
“In 1997, several doctors were accused of homicide for discontinuation of the artificial respirator, even though there was no possibility of survival. Since this case, lots of terminal patients have had a meaningless life prolonged against their will and their family’s requests,” said Park. “A concrete law about euthanasia is needed to avoid unnecessary conflict between doctors’ legal obligations and clients’ free will.”
But the question of what constitutes free will is not necessarily always straightforward. Ku In-hoe, director of the Catholic Institute of Bioethics at The Catholic University of Korea, raised concerns that the proposed law could be abused by people hoping to manipulate patients in a vulnerable position.
“This proposed recommendation categorized ‘canceling life-prolonging treatment by the patient’s own will’ into three cases. There is the risk of abusing the law or violating basic civil rights when the patient’s own will is unclear. If the decision is made only based on testimonies by third persons, such as the doctors, family members or an attorney, the patient’s own will may be distorted,” said Ku. “For example, family members may distort the decision due to their financial burden or inheritance problems. Therefore, extra safety measures should complement such loopholes in the law.”
Lee In-jae, an ethics professor at Seoul National University of Education, also warned of the potential for such abuse.
“I think the laws allowing euthanasia are likely to be used for evil,” said Lee. “(Such as) in cases where a patient’s family gives priority to money ― treatment cost ― more than the patient’s life and the hospitals want to get human organs more easily. So the laws (need) to have more detailed and strict limitations in order to protect the patient’s dignity and life.”
But even if a patient’s decision is his own, questions remain about the mental state of those who wish to die. In the proposal put forward last month, two doctors, one specialist and one general physician, would be required to sign off on a patient’s decision to forgo treatment. In his opinion as a mental health professional, however, Park said that a psychiatrist’s assessment of patients refusing treatment would be crucial to the implementation of any new regime.
“Psychiatric assessment of mental state, especially competence, is required before a decision of ‘do not resuscitate’ or euthanasia based on free will,” said Park. “I think that at least two different psychiatrists of another hospital or an independent committee should agree on a patient’s competence and judgment through careful interviews with the patient by themselves and their family members. If the patient’s ability of judgment is equivocal, the request for euthanasia should be dismissed.”
Philosophical objections
Nevertheless, a clean bill of mental health is unlikely to assuage all concerns about moves to loosen the law. Philosophical or religious objections mean that free will is far from the start and end of the debate.
“The free will of human beings certainly needs to be respected, but the responsibility of human life is the first priority,” said Ku. “Free will only works with the premise that the concerned person is alive. Considering the fact that harming others’ life is a crime, harming one’s own life cannot be a righteous way of exercising one’s civil rights.”
By John Power (john.power@heraldcorp.com)
Yoon Ha-youn contributed to this report. ― Ed.
Readers’ voice
Euthanasia...
This is a controversial issue around the world. However, in my opinion, it depends on the serious situations the patients go through. There have been a lot of miracles happening to people suffering from incurable diseases who survive. This shows as long as you have faith in those who can get over difficulties they are going through, you should wait and support them, because people’s lives are valuable and we do not have any permission to take their lives. Yet, this requires a lot of sacrifice from the patients and people who support them. Moreover, this may be harder for the sufferers to fight with themselves and make their families wait for a long, undetermined period of time until they wake up. I think what the best solution for both of them is to let the sufferers stop suffering by euthanasia and pray for them to live in heaven with better circumstances.
― Bobby Tek, Albury, Australia
It should be legalized out of basic human compassion and respect for the terminally ill. Each case should require maybe three different doctors’ diagnoses of the terminal nature of the illness, and it should be guaranteed that those consultations will be made promptly. I would like to have the right to die humanely if I were in such a condition, rather than be faced with suicide as the only way to avoid prolonged and pointless suffering.
― Audwin Wilkinson, Jeungpyeong, North Chungcheong Province
Cost of sporting events...
One of the biggest issues Korea has had is in assuming the people will come instead of doing a full-on ROI analysis. There’s also the lack of accountability ― it’s not their money, so what do we have to lose?
― Chris Backe, Bangkok, Thailand, via Facebook
Actually some local governments are attracting such events without a big enough budget. They think the central government will support the event if it’s an international event. They think that they can make some infrastructure with support from the central government, and in that case it is worth it, even if the event itself shows a loss.
― Jung Un-soo, Seoul, via Facebook

-
Articles by Korea Herald



















![[Today’s K-pop] Treasure to publish magazine for debut anniversary](http://res.heraldm.com/phpwas/restmb_idxmake.php?idx=642&simg=/content/image/2024/07/26/20240726050551_0.jpg&u=)