Terminally ill patients who have no other medical options but to hang on to life with essential treatment will likely be given the right to die starting next year.
A subpanel of the presidential committee on bioethics has reached an agreement to legally allow patients who are dying or their families to decide whether to withdraw treatment that is keeping them alive.
According to the subpanel’s advisory report released by the Ministry of Health on Monday, a terminal patient can voluntarily forgo life-sustaining treatments by stating how they want to be treated if they can no longer make health care decisions for themselves.
The committee suggested documenting their will through “advance directives” and “physician orders for life-sustaining treatment,” so that doctors could stop providing treatments as the patients wished. Life-sustaining care includes CPR, artificial respiration, blood filtration and the use of anti-cancer drugs.
However, drugs to control pain, nutrition, water and oxygen should be provided. The new rule will be put under discussion at a plenary meeting of the National Bioethics Committee next week. It is likely to be submitted to the health ministry in June and also legislated by the end of the year if it gets parliamentary approval. The plan is expected to go into effect next year at the earliest.
A subpanel of the presidential committee on bioethics has reached an agreement to legally allow patients who are dying or their families to decide whether to withdraw treatment that is keeping them alive.
According to the subpanel’s advisory report released by the Ministry of Health on Monday, a terminal patient can voluntarily forgo life-sustaining treatments by stating how they want to be treated if they can no longer make health care decisions for themselves.
The committee suggested documenting their will through “advance directives” and “physician orders for life-sustaining treatment,” so that doctors could stop providing treatments as the patients wished. Life-sustaining care includes CPR, artificial respiration, blood filtration and the use of anti-cancer drugs.
However, drugs to control pain, nutrition, water and oxygen should be provided. The new rule will be put under discussion at a plenary meeting of the National Bioethics Committee next week. It is likely to be submitted to the health ministry in June and also legislated by the end of the year if it gets parliamentary approval. The plan is expected to go into effect next year at the earliest.
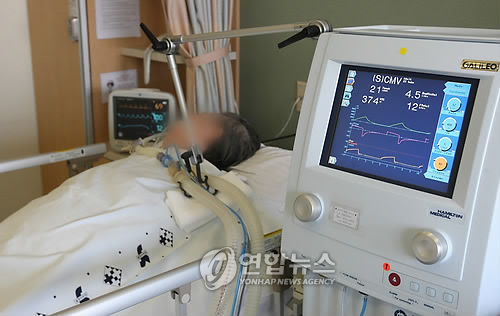
The plan, however, is likely to stir controversy as many Koreans believe the concept of withdrawing life-supporting care is abandoning life.
Huh Dae-seok, a medical professor at Seoul National University, said Koreans are “obsessive with medical technology” and “in denial of the concept of well-dying.”
“People don’t understand how painful the life-sustaining treatment is. It is a meaningless and unnecessary procedure that would prolong just a few days for the patients who are already in the dying process,” he said in an interview with The Korea Herald.
According to the Health Ministry, about 250,000 Koreans die every year and most of them end their lives in hospitals. The ministry assumes that from the number of death in Korea about 30,000 patients took life-suspending treatments. More than 30 percent of cancer patients received chemotherapy a month before they died, National Cancer Center said.
Even calling it “meaningless” and “futile,” doctors and hospitals have been providing treatments because they are legally bound to do so.
In Germany and Austria, doctors are not allowed to provide medical treatment against the will of the patients, Korean doctors would face a jail term if they do not perform necessary treatments.
The new rule drafted by the subpanel states that life-support can be ended with the patient’s family’s consent, if he or she is in coma and thus cannot make the decision. The decision requires all family members’ agreement as well as from two doctors.
Due to the family-oriented culture in Korea that puts a greater value on filial duty, it will be hard for families to make the decision even if they understand the procedure is “meaningless.”
“They don’t want to be blamed by others that they made such decision that killed their parents or other family members,” Huh said.
Due to this peculiar culture, legalizing the right to die likely has a bumpy road ahead. Some lawmakers have proposed so-called “death with dignity” bills in recent years, but they have never even made it to a plenary session as they failed to get public support.
Granting the right to hospital ethics committees to end treatments for comatose patients who have no family is also likely to open up ethical concerns.
The Catholic Church in Korea has also been voicing its opposition to the plan to allow surrogate decisions, saying it devalues the human life and could be abused for unethical purposes.
Ku In-hoe, a professor at the Catholic University of Korea, said the Catholic Church is concerned about the plan because it could justify controversial choices such as euthanasia and physician-assisted suicide.
“Legalizing (the patients’ right to withdraw end-of-life care) could cause unprecedented results in a society that has not fully embraced the great value of human life yet. Even if the plan is to reduce the financial burden (on patients and their families), the plan would violate the dignity of a man,” she said.
The plan could also throw families into chaos if they fail to make the decision unanimously.
“It has to include specific rules for families who have different ideas such as utilizing hospital ethics committees that are consisted of doctors, religious figures and scholars on bio ethics,” she added.
Citing the gravity of the issue, experts added that the government needs to seek social consensus and establish another legal tool to monitor the plan so that it is not being misused.
Legalizing the right to die for terminally ill patients has sparked a heated debate since the late 1990s.
The issue was first brought up to the public when a court convicted a family of murder and a doctor of assisting them for removing a ventilator from a comatose patient.
In 2009, the Supreme Court ruled to have life support removed from a 75-year-old patient in a coma. It was reported as the country’s first “death with dignity” case. The court’s decision was based on the assumption that the patient would have refused to have life-suspending treatment if she was still awake, based on her usual remarks and values.
By Cho Chung-un (christory@heraldcorp.com)
-
Articles by Korea Herald











![[Hello India] Hyundai Motor vows to boost 'clean mobility' in India](http://res.heraldm.com/phpwas/restmb_idxmake.php?idx=644&simg=/content/image/2024/04/25/20240425050672_0.jpg&u=)








