CHICAGO (AP) ― Many breast cancer patients can skip aggressive lymph node surgery without increasing their chances of a recurrence or death if their disease shows limited spread, according to a study that has prompted changes in practice.
Under current guidelines, the often-debilitating surgery is done if the cancer has spread outside the breast to any lymph nodes.
In the study, rates of survival and of patients’ remaining cancer-free were just as good whether the women with limited spread ― in one or two nearby nodes ― had lots more underarm nodes removed or skipped that major surgery.
At least 24,000 of the 180,000 U.S. women diagnosed every year with breast cancer have limited spread to lymph nodes. Under the standard approach, they would have a chunk of underarm tissue removed to check for further cancer spread, said Dr. Thomas Julian, a breast cancer specialist with West Penn Allegheny Healthcare System in Pittsburgh. He was not involved in the study.
That operation often leaves women with lasting arm swelling, stiffness and pain.
The results suggest that tens of thousands of women could be spared aggressive node surgery and those troubling side effects, said study author Dr. Armando Giuliano, cancer surgery chief at the John Wayne Cancer Institute in Santa Monica, California
“This is really a move toward less radical surgery” for breast cancer patients, he said.
Under current guidelines, the often-debilitating surgery is done if the cancer has spread outside the breast to any lymph nodes.
In the study, rates of survival and of patients’ remaining cancer-free were just as good whether the women with limited spread ― in one or two nearby nodes ― had lots more underarm nodes removed or skipped that major surgery.
At least 24,000 of the 180,000 U.S. women diagnosed every year with breast cancer have limited spread to lymph nodes. Under the standard approach, they would have a chunk of underarm tissue removed to check for further cancer spread, said Dr. Thomas Julian, a breast cancer specialist with West Penn Allegheny Healthcare System in Pittsburgh. He was not involved in the study.
That operation often leaves women with lasting arm swelling, stiffness and pain.
The results suggest that tens of thousands of women could be spared aggressive node surgery and those troubling side effects, said study author Dr. Armando Giuliano, cancer surgery chief at the John Wayne Cancer Institute in Santa Monica, California
“This is really a move toward less radical surgery” for breast cancer patients, he said.
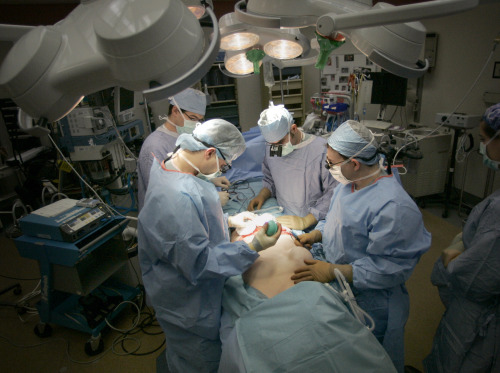
That move began several years ago when doctors stopped routinely removing entire breasts and surrounding tissue, except for women with more advanced disease.
The study refutes previous research suggesting a greater chance for recurrence when cancer is found in one or two nodes.
The difference may be the overall treatment given to the women in the study.
All had relatively early disease, with spread to no more than two nodes. They were treated with lumpectomies to remove their tumors and a common type of radiation that covers the breast and underarm area. Most also had chemotherapy, hormone treatment, or both.
American Society of Surgical Oncology guidelines recommend aggressive node surgery for such women. The group is doing a periodic guideline review, and the study results likely will lead to some changes, said Dr. Gary Lyman of Duke University, co-chair of a panel involved in those guidelines.
“This certainly is a pivotal study and an important additional piece of information in an area that we’ve been waiting for,” Lyman said.
The study appears in Wednesday’s Journal of the American Medical Association. Some details were presented at a medical meeting last year and led many doctors to adopt the new approach. That includes breast surgeons at New York’s Memorial Sloan-Kettering Cancer Center and the M.D. Anderson Cancer Center in Houston, according to study co-authors from those institutions.
The results confirm the approach is safe, and doctors can feel confident recommending it, said Dr. Nora Jaskowiak, surgical director of the breast center at University of Chicago Medical Center.
The study involved about 850 women who had initial biopsies showing cancer had spread to one or two nearby lymph nodes.
Lymph nodes are tiny structures linked by a network of vessels throughout the body that are part of the disease-fighting immune system. When cancer spreads, it typically travels first to nearby nodes.
About half of the women were randomly assigned to receive the more invasive node surgery; the remainder skipped that surgery.
Roughly 92 percent in both groups were still alive five years later, and 83 percent in both groups had no cancer recurrence. Seventy percent of women in the surgery group had complications, including underarm swelling and wound infection, versus 25 percent in the group that skipped it.
Julian, the Pittsburgh breast surgeon, said there were limitations to the research, including how women were recruited.
The researchers approached women who already knew their initial lymph node biopsy results, and only about half as many women as anticipated agreed to be in the study. Higher-risk women who wanted conventional node surgery may have chosen not to participate, which could have skewed the results.
The study authors acknowledge that limitation but said even high-risk study participants, those with breast cancer that does not respond to hormone treatment, had good long-term survival rates even without the node surgery.
Julian said lack of extended follow-up is also a concern.
“You need to have 10 years to really know that it’s going to hold water,” he said.
He said he has cautiously adopted the study approach with older patients, but only on a case-by-case basis with women 50 or younger, who have longer to live and more time for cancer to recur.






![[KH Explains] How should Korea adjust its trade defenses against Chinese EVs?](http://res.heraldm.com/phpwas/restmb_idxmake.php?idx=644&simg=/content/image/2024/04/15/20240415050562_0.jpg&u=20240415144419)